Understanding Sensory Processing in Children with Autism: A Parent’s Guide
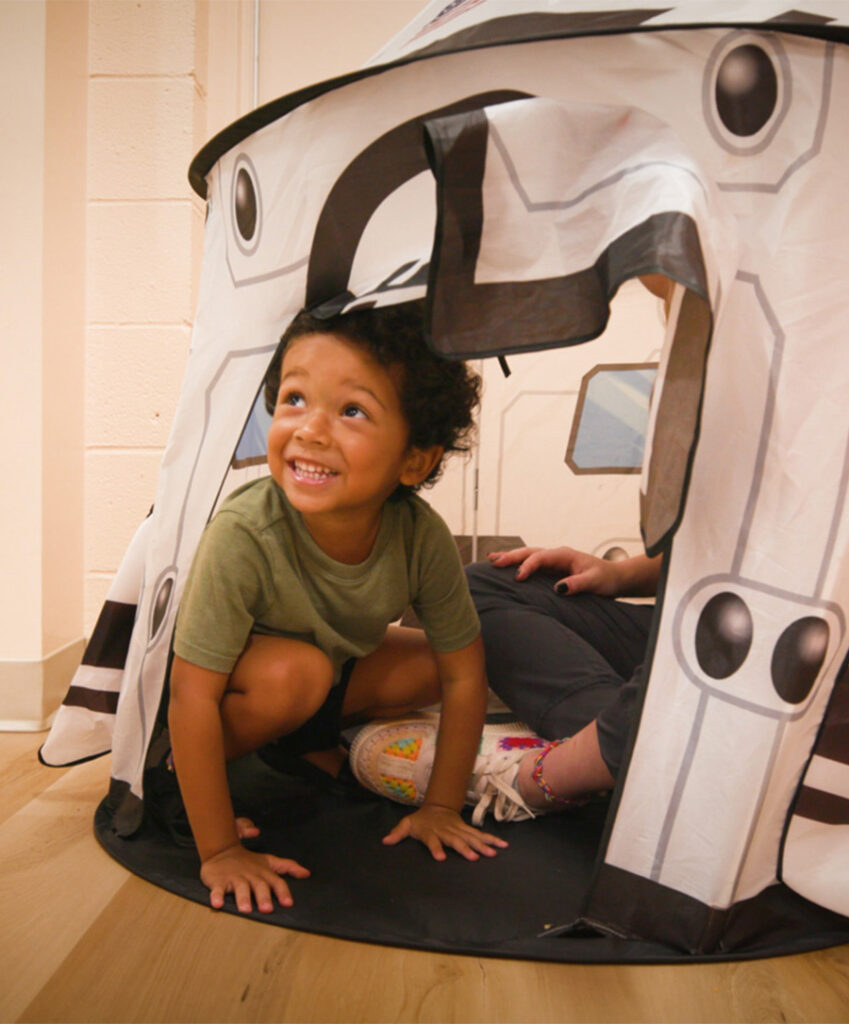
Your child covers their ears when the school bell rings. They melt down at the grocery store but seem perfectly calm at home. They won’t wear certain clothes or eat particular textures. These reactions often mystify parents, why is your child so sensitive to things that other kids don’t seem to notice?
Welcome to sensory processing differences, one of the most challenging yet least understood aspects of autism. At Children’s Specialized ABA, we work with families throughout New Jersey, in Jackson, Clifton, and beyond, helping them understand what sensory processing is, why it matters, and how to support their child’s regulation and development.
What Is Sensory Processing?
Sensory processing is the brain’s ability to take in sensory information, light, sound, touch, taste, smell, movement, and body awareness, organize it, and respond appropriately. For neurotypical children, this happens largely automatically. They hear a fire alarm, their brain recognizes it as loud but temporary, and they carry on. For many children with autism, sensory processing works differently.
A child with sensory processing differences might experience the same fire alarm as overwhelming, distressing, or even painful. Their nervous system may amplify certain sensations while filtering out others. This isn’t a choice, a behavioral problem, or a phase. It’s how their brain is wired.
Sensory processing differences fall into a few broad categories:
Sensory sensitivity (hypersensitivity): The child’s nervous system amplifies certain sensations. Loud noises feel painfully loud. Light textures feel irritating. Strong smells are nauseating. The tag in a shirt isn’t a minor annoyance, it’s genuinely distressing.
Sensory seeking (hyposensitivity): The child’s nervous system under-registers certain sensations, so they seek more input. They crave deep pressure, spin repeatedly, seek out loud noises, or eat non-food items. These behaviors are attempts to get their sensory system stimulated enough to feel regulated.
Sensory avoidance: The child actively avoids certain sensations. They refuse to walk in sand, avoid playgrounds with certain surfaces, resist getting their hands messy, or refuse to touch certain textures. What looks like stubbornness is often genuine distress avoidance.
Many children experience a mix of all three, hypersensitive to sound but hyposensitive to pain, seeking deep pressure while avoiding light touch. Understanding your child’s unique sensory profile is the first step toward helping them.
How Sensory Processing Affects Daily Life
At School
A child who is hypersensitive to sound might be overwhelmed by the cafeteria (noisy, echoing), transitions between classes (hallway chaos), or the sound of pencils on paper. The classroom feels like sensory assault. By the time they get home, they’re dysregulated and exhausted from managing their sensory system all day, leaving little capacity for homework or family interaction.
A child who is sensory seeking might need to fidget constantly, rock in their chair, or create stimulation that the teacher perceives as disruptive. They’re not trying to be difficult, they’re trying to regulate their nervous system so they can learn.
At Home
Family mealtimes become battles. Your child will eat only specific textures (chicken nuggets, white rice, applesauce) and refuses everything else. It’s not pickiness, the other foods genuinely feel wrong in their mouth. Getting dressed becomes a meltdown. Bedtime is hours of resistance because their pajamas feel wrong or the room is too bright.
In the Community (Jackson, Clifton, and Throughout New Jersey)
A trip to the grocery store becomes a sensory nightmare. The fluorescent lights, the beeping of the scanner, people touching your child, the smell of the deli counter, the overwhelming number of visual stimuli, your child shuts down or explodes. What should be a simple errand becomes a stressful ordeal, and you find yourself leaving events early or avoiding outings altogether.
Birthday parties, restaurants, parks, and family gatherings all become situations you dread because you can’t predict whether your child will be regulated or dysregulated.
The Regulation-Behavior Connection
Here’s a critical insight that changes how you understand your child’s behavior: most challenging behaviors in children with autism are, at their root, regulation difficulties. A child isn’t being defiant when they refuse to transition. They’re dysregulated by the sensory chaos of the transition. A child isn’t being aggressive when they hit during a meltdown. Their sensory system is overwhelmed and they don’t have the tools to manage it.
This is crucial: when you understand behavior as a symptom of sensory dysregulation, you stop viewing your child as difficult and start viewing them as struggling. This shift in perspective changes everything about how you respond.
Practical Strategies for Supporting Sensory Regulation
1. Create a Sensory Profile
Before you can help, you need to understand. Over the next week, notice your child’s reactions. When are they most dysregulated? What sensations seem to bother them? What do they seek out? Do they crave heavy pressure? Do they avoid certain textures? Keep a simple log:
- Situation: What was happening when dysregulation occurred?
- Sensory trigger: What sensory input might have caused it?
- Response: How did your child respond?
- What helped: What calmed them down?
Over two weeks, patterns emerge. You’ll notice your child is always upset during loud environments, or that deep pressure (hugs, weighted blankets) calms them, or that they can’t tolerate seams on socks. This is your child’s sensory map.
2. Modify the Environment
You can’t change your child’s sensory nervous system, but you can change the environment they’re experiencing. Some practical modifications:
For sound sensitivity: Use noise-canceling headphones at loud events (you’d be surprised how many schools and public places allow this). Create a quiet space at home where your child can retreat. Use softer background music instead of television. Warn your child before loud events (“The fire alarm will go off at 10:00. It will be very loud for about 30 seconds, then it will stop.”) so they’re not surprised.
For light sensitivity: Install softer, warmer lighting. Reduce screen time before bedtime. Allow your child to wear sunglasses outdoors if it helps. Use blackout curtains in bedrooms. Some children benefit from dimmer switches.
For touch sensitivity: Wash all new clothes before wearing. Cut out tags. Choose clothing with no seams, no itchy materials. Let your child choose their clothes when possible (within appropriate boundaries) so they have control. Avoid unexpected touches, ask before hugging.
For taste and smell sensitivity: Don’t force new foods. Serve familiar foods alongside new ones with no expectation of trying. Allow your child to wear a scarf or mask if strong smells are distressing. Prepare foods without visible pieces (smooth peanut butter instead of chunky) if your child is texture-averse.
3. Provide Sensory Input on Your Child’s Terms
Children who are sensory seeking need appropriate outlets. Instead of suppressing the need, channel it:
For movement seeking: Provide a trampoline, swing set, or access to running and jumping. Let your child spin if it helps them regulate (in a safe space). Dance together. Use a treadmill or exercise bike.
For pressure seeking: Use weighted blankets, weighted vests, or weighted lap pads. Create “sandwich” activities where you place pillows on top of your child and press gently. Allow your child to burrow under couch cushions. Use tight hugs with their permission.
For oral seeking: Provide chewing gum, chewy snacks, crunchy foods, hard candies, or chewy toys. A child who chews on their clothes isn’t trying to be difficult, they’re seeking oral input. Provide acceptable alternatives.
4. Teach Your Child to Communicate Their Needs
A child who can’t tell you that the lighting is uncomfortable or that the tag is bothering them will act out instead. Start teaching sensory awareness and communication early:
- Use visual supports: Show pictures of ears (hearing), eyes (seeing), skin (touch), mouth (taste), nose (smell)
- Use simple language: “Your ears are hearing loud sounds” instead of expecting them to label it themselves
- Create a sensory communication board: Pictures of different sensory experiences with simple words
- Validate their experience: “The light is bright and that’s bothering you. Let’s find a quieter place”
- Eventually, with practice, your child can learn to communicate: “I need quiet” or “This is itchy”
5. Prepare, Prepare, Prepare
Surprises are sensory nightmares. A child doesn’t know what sensory input is coming, so they can’t prepare their nervous system. Advance warning helps tremendously:
- Before going to the grocery store: “We’re going to the store. It will have bright lights and noises from the scanner and people. You can wear your headphones”
- Before a haircut: Visit the salon first without cutting to see it. Watch videos of haircuts. Let your child wear headphones during the actual cut
- Before a family event: “Grandma’s house has a lot of people and noise. You can take breaks in the bedroom if you need to”
- Before school transitions: Give a 5-minute warning before transitions, then a 2-minute warning
Predictability reduces anxiety and dysregulation dramatically.
Red Flags: When to Seek Professional Help
Some sensory differences are minor and manageable with environmental modifications. Others significantly impair your child’s functioning and quality of life. Seek professional evaluation if:
- Your child is frequently dysregulated or melting down
- Sensory sensitivities are preventing school attendance or social participation
- Your child is self-injuring (hitting themselves, head-banging) when dysregulated
- Feeding difficulties are resulting in nutritional deficiency or feeding tube dependency
- Your child cannot participate in daily routines (dressing, bathing, grooming) due to sensory aversion
- You’re unsure whether your child’s sensitivities are typical or warrant intervention
What Professional Treatment Looks Like
Occupational Therapy (OT)
An occupational therapist specializes in sensory processing and regulation. They can:
- Conduct a formal sensory assessment to identify your child’s specific profile
- Create a “sensory diet”, a personalized plan of sensory activities throughout the day to keep your child regulated
- Teach your child body awareness and regulation strategies
- Work with you on environmental modifications and daily routine adaptations
- Provide sensory-motor activities that build coordination and reduce dysregulation
ABA Therapy
Applied Behavior Analysis can address the behavioral consequences of sensory dysregulation. An ABA therapist working with your child at one of our New Jersey locations (Jackson, Clifton, and beyond) can:
- Help your child learn regulation strategies before they become dysregulated
- Teach communication skills so your child can express sensory needs instead of acting out
- Create a systematic plan for reducing avoidance behaviors (like refusing to wear socks) through gradual exposure and reinforcement
- Work on transitions, which are major sensory challenges for many children
- Provide data on which sensory modifications and strategies actually work for your specific child
The Combination Approach
Many children benefit from both OT and ABA working together. OT addresses the sensory system itself; ABA addresses the behaviors and skills that help your child function despite sensory challenges. Parents guide the system by providing consistent, predictable routines and environmental supports at home and in the community.
What Therapy Looks Like: A Real Example
Sarah, age 8, refuses to eat anything except white foods (chicken, rice, applesauce, bread). Her parents have tried pressuring her, negotiating, hiding other foods in her meals, nothing works. She’s lost weight and they’re concerned about nutrition.
Her OT assessment revealed she’s hypersensitive to taste and texture. Her tongue registers normal foods as unpleasantly intense. For her, trying a piece of pizza is genuinely distressing, it’s not stubbornness.
Her OT created a “sensory diet” that includes oral input activities (crunching hard foods, chewing gum, sucking on ice) to help Sarah’s taste system feel less overwhelmed. Her ABA therapist worked on systematic food exposure: starting with foods that smell similar to her safe foods, then similar colors, then slightly different textures. Not through pressure or punishment, but through a gradual plan where Sarah learns to tolerate new foods with support.
Her parents modified their home: served meals in a quiet space (not with the TV on), offered cold foods (which are sometimes easier for sensitive kids), and stopped pressuring her. Within four months, Sarah was eating five new foods and her anxiety around mealtimes had dropped significantly.
Parent Self-Care: You’re Allowed to Be Tired
Managing a child with significant sensory processing differences is exhausting. You can’t take them to restaurants. You can’t do typical playdates. Vacations require extensive planning. Your own sensory needs often go unmet while you’re managing theirs.
This is real. Your exhaustion is valid. You’re not failing if you sometimes find it all overwhelming. You’re human.
Build in supports for yourself: respite care, support groups where you can talk with other parents who understand, therapy for yourself if you need it, and grace for the days when you just can’t be perfect. You can’t regulate your child if you’re dysregulated.
The Long View: Development Over Time
Sensory processing differences don’t disappear, but they do evolve. A toddler with sound sensitivity might become a school-age child who can tolerate some noise with headphones. A teenager might develop their own regulation strategies. An adult might structure their life around their sensory needs (choosing a quiet job, living in a quiet neighborhood, controlling their environment).
The goal isn’t to “fix” your child’s sensory system. It’s to help them understand themselves, develop strategies, and live as comfortably and independently as possible within their neurological reality.
When to Start: Early Intervention Matters
If your child is under age 3 and showing signs of sensory processing differences or autism, contact your state’s early intervention program immediately. Early intervention services (often free or low-cost) can provide OT and other services before your child starts school.
If your child is school-age, request an evaluation through your school district’s special education process. Schools are required to provide OT and other services if sensory processing issues are impacting your child’s education.
If you’re seeking services in New Jersey (Jackson, Clifton, and throughout the state), Children’s Specialized ABA can help coordinate care and provide ABA services that work in concert with your child’s occupational therapy and school services.
Moving Forward: You’re Not Alone
If your child is showing signs of sensory processing difficulties, you’re likely feeling confused, frustrated, or scared. You’re wondering if you’re doing something wrong. You’re not. Your child’s sensory processing differences are neurological, not parental.
What you can do is understand your child, modify their environment, teach them strategies, and connect them with professionals who can help. You can celebrate their unique sensory experience while helping them function in a world that wasn’t designed with their sensory needs in mind.
At Children’s Specialized ABA, we’ve supported hundreds of families throughout New Jersey, in Jackson, Clifton, and communities across the state. We know that children with sensory processing differences are often incredibly thoughtful, creative, and perceptive. Their sensitivity is part of their gift. The goal is helping them manage that sensitivity so it doesn’t prevent them from living their best life.
If you have questions about sensory processing, or if you’d like to discuss whether ABA therapy might help your child, we’re here. Call us or visit our website to learn more about our services for children with autism and sensory processing differences.
Your child’s sensory experience is real. Your efforts to support them matter. You’re doing better than you think.